If you live with hypermobile Ehlers-Danlos syndrome (hEDS), POTS, or mast cell activation syndrome (MCAS), you may already know this experience well.
You’re unwell.
Your symptoms are real.
But your blood tests come back “normal”.
For many people with complex, multisystem conditions, standard testing doesn’t capture what’s actually happening inside the body, especially during flares. And when results don’t match lived experience, trust can quietly erode.
The problem isn’t testing. It’s how and when we test.
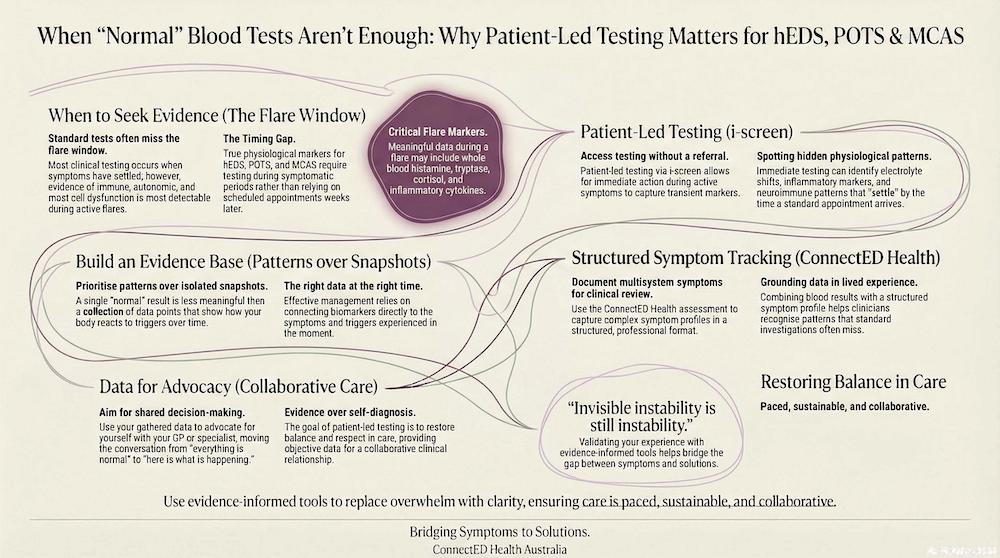
In recent years, independent blood testing has become more accessible. Much of the mainstream conversation focuses on:
- How many biomarkers are included
- Whether results are “AI-analysed”
- How detailed or polished the report looks
But for people with hEDS, POTS and MCAS, those aren’t the real differentiators.
What matters more is:
- Timing: testing during flares, not weeks later
- Relevance: markers linked to immune, autonomic and mast cell activity
- Context: patterns over time, not isolated snapshots
- Interpretation: connecting results back to symptoms, not just ranges
More data doesn’t automatically mean better care. The right data, at the right time, does.
Why “comprehensive” testing often misses the point
Many blood testing services advertise “comprehensive panels”, but there’s no universal definition of what that actually means.
Often, large biomarker counts include a mix of:
- Raw biomarkers (directly measured), and
- Calculated markers (ratios or indexes derived from existing results)
That distinction matters, but for complex conditions, it’s only part of the picture.
A test can look comprehensive on paper and still miss the markers that matter for:
- Mast cell activation
- Autonomic stress responses
- Electrolyte shifts
- Inflammatory or neuroimmune patterns
If those markers aren’t included, or if testing only happens when symptoms have settled, results can feel invalidating rather than helpful.
Patient-led testing changes the power dynamic
This is where patient-led testing, such as i-screen, becomes meaningful.
Instead of waiting for referrals or trying to time tests around a “good day”, patient-led testing allows you to:
- Test when symptoms are active
- Choose tests relevant to your condition
- Build a pattern over time, rather than relying on a single result
- Take objective data back to your GP or specialist
At ConnectED, we see this as a shift from chasing diagnoses to building evidence.
Not to self-diagnose.
Not to replace clinicians.
But to restore balance, respect, and collaboration in care.
How i-screen fits into patient-led testing for hEDS, POTS & MCAS
Patient-led testing works best when it’s intentional, not random.
For people living with hEDS, POTS and MCAS, symptoms fluctuate, and standard testing often misses the window where meaningful changes are happening. This is where i-screen testing can be particularly useful.
Based on ConnectED’s patient guide, i-screen testing is most effective when organised into three clear purposes rather than a single “one-size-fits-all” panel .
1. Baseline testing (when you are relatively stable)
This establishes a reference point for your body outside of acute flares. Common baseline tests may include:
- Full blood count with differential
- Electrolytes and kidney function
- Liver function
- Iron studies and ferritin
- Active B12, folate and vitamin D
- Thyroid markers
Baseline results don’t always explain symptoms, but they provide essential context for what comes next.
2. Flare testing (when symptoms are active)
This is where patient-led testing can be transformative.
Instead of waiting weeks for an appointment after a flare has passed, i-screen allows testing during symptomatic periods, helping capture neuroimmune and autonomic stress signals such as:
- Mast cell markers (e.g. whole blood histamine, tryptase)
- Cortisol and inflammatory cytokines
- Electrolyte shifts linked to POTS symptoms
- Metabolic and neurotoxin stress pathways
This approach can directly link flare symptoms to measurable biomarkers, something that is rarely possible in standard care models .
3. Maintenance and nutritional monitoring
Over time, repeat testing can support longer-term management by tracking:
- Intracellular minerals (e.g. RBC magnesium)
- Nutrients involved in connective tissue and mast cell stability
- Mitochondrial and metabolic markers
- Gut and nutrient demand patterns
Used thoughtfully, this helps identify trends rather than chasing isolated “out of range” results.
Importantly, i-screen testing is patient-led. You don’t need a GP referral to order tests, and results can be taken directly to your doctor or specialist to support shared decision-making.
If you’d like to explore this approach, you can access i-screen here.
Testing alone isn’t the answer, but when combined with symptom tracking, clinical care and lived experience, it can become a powerful advocacy tool.
Where the ConnectED Health assessment fits
Testing is most useful when it’s guided by a clear understanding of your symptom patterns.
This is where the ConnectED Health assessment complements patient-led testing.
The assessment helps you:
- Capture multisystem symptoms in a structured way
- Identify patterns commonly seen in hEDS, POTS and MCAS
- Generate a clear report you can share with your doctor
- Use your symptom profile to inform more targeted conversations about testing and care
When symptom data and blood test results are viewed together, patterns are often easier to recognise, particularly in conditions that don’t show up clearly in standard investigations.
The ConnectED Health assessment is available on the Apple App Store and Google Play.
It’s designed to support clinical conversations, not replace them, and to help patients advocate with clarity rather than overwhelm.
AI reports aren’t the answer, understanding is
Many platforms now offer AI-generated summaries and “personalised insights”. These tools can be useful for organising information, but they are not a substitute for:
- Condition-specific knowledge
- Lived experience
- Clinical reasoning
- And a healthcare professional who understands context
For complex conditions, the real value lies in connecting the dots:
- Symptoms
- Biomarkers
- Triggers
- Flares
- Recovery patterns
That connection happens when data is grounded in real human experience.
From symptoms to solutions: one step at a time
For people living with hEDS, POTS and MCAS, progress is rarely linear. Care works best when it is:
- Patient-led
- Evidence-informed
- Collaborative
- And paced for sustainability
Testing and assessment are not endpoints. They are tools, part of a broader picture.
When used thoughtfully, they can help shift conversations from:
“Everything looks normal”
to
“Here’s what’s happening — and here’s how we move forward.”
Medical Disclaimer
This content is for informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your doctor or qualified health provider regarding any medical condition.
FAQ
What is Hypermobile Ehlers-Danlos Syndrome misdiagnosis?
It’s when hEDS symptoms are mistaken for other conditions like anxiety, depression, or IBS, delaying correct treatment.
Why is hEDS often misdiagnosed?
Because it affects multiple systems and lacks a definitive test, symptoms can resemble unrelated physical or mental health conditions.
How long does it take to get diagnosed with hEDS?
On average 10–12 years, sometimes longer, due to low awareness among healthcare providers.
Can the ConnectED Health App help my doctor diagnose hEDS?
While not a diagnostic tool, it provides a structured symptom report to support the diagnostic
process.
What other conditions are linked with hEDS?
Common overlaps include POTS, MCAS, neurodivergence, and post-viral syndromes like Long COVID.
About the Author
Tracy Finnegan, RN, BAppSc is the Founder and Managing Director of ConnectED. A former ICU nurse and scientist, Tracy has lived experience with hEDS, POTS, MCAS, and Long COVID. After decades of misdiagnoses, she created the ConnectED Health App to empower patients to track symptoms, identify patterns, and advocate for accurate diagnoses and better care. Tracy brings firsthand experience, clinical expertise, and a patient-focused tool to support others.


