Understanding the Different Phenotypes of Hypermobile Ehlers-Danlos Syndrome (hEDS)
What is hEDS? Hypermobile Ehlers-Danlos Syndrome (hEDS) is a complex condition that affects the body’s connective tissue—the “glue” that holds everything together. Connective tissue supports skin, joints, blood vessels, and even the nervous and immune systems. People with hEDS often experience joint pain, stretchy skin, and frequent injuries, but symptoms can go far beyond the joints.
Our Theory: Different Phenotypes, Different Experiences
Based on years of clinical observation, personal experience, and genetic research, we believe that hEDS doesn’t present the same way in everyone. Instead, it may express itself through distinct phenotypes, or patterns of symptoms. These patterns reflect which systems in the body are most affected. Understanding a person’s unique phenotype could help guide better diagnosis and treatment.
We’ve grouped hEDS into five main phenotypes:
1. Musculoskeletal Phenotype
- What it looks like: joint hypermobility, chronic pain, frequent subluxations or dislocations, scoliosis, early onset osteoarthritis
- Common symptoms: clicking joints, poor posture, fatigue from joint instability, slow injury healing
- Genetic overlaps: COL5A1, TNXB, other collagen-related genes
2. Cardiovascular Phenotype
- What it looks like: heart palpitations, fainting when standing (POTS), low blood pressure, stretchy or fragile blood vessels
- Common symptoms: dizziness, cold hands and feet, fast heart rate, migraines
- Genetic overlaps: variants in autonomic nervous system regulation, adrenergic receptor genes
3. Cystic Phenotype
- What it looks like: formation of cysts, abnormal fluid retention, recurring infections in glands (e.g., sinuses, trachea, breasts), endometriosis, PCOS
- Common symptoms: bloating, hormone imbalances, acne, skin cysts, pilonidal sinus (especially in males)
- Genetic overlaps: CFTR variants (cystic fibrosis-related genes), hormone metabolism genes
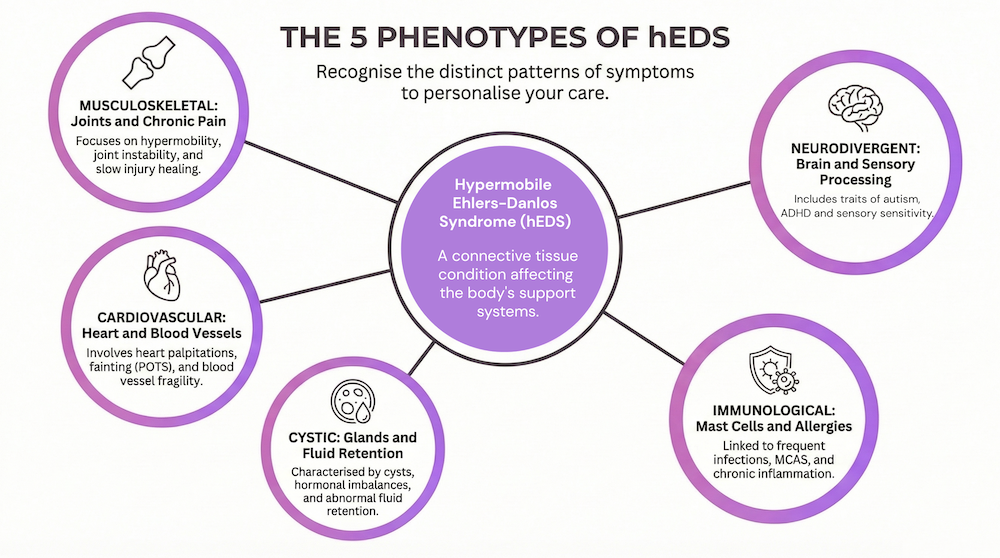
4. Immunological Phenotype
- What it looks like: frequent infections, allergies, Mast Cell Activation Syndrome (MCAS), autoimmune-like symptoms
- Common symptoms: hives, flushing, food sensitivities, asthma, chronic inflammation
- Genetic overlaps: immune regulation genes, cytokine signaling, mast cell function
5. Neurodivergent Phenotype
- What it looks like: traits of Autism Spectrum Disorder (ASD), ADHD, sensory sensitivities, emotional regulation challenges
- Common symptoms: overwhelm in noisy environments, difficulty focusing, stimming behaviors, sleep disturbances
- Genetic overlaps: CNTNAP2, SHANK2, ALDH7A1 (related to B6 metabolism), dopamine and serotonin pathway genes
A Mixed Bag? Many people with hEDS experience a combination of these phenotypes. That’s totally normal—these groupings are not strict boxes, but tools to help understand why symptoms vary so much from person to person.
What Does This Mean for You? By identifying your dominant phenotype(s), you and your healthcare provider might be better equipped to:
- Understand your body’s unique needs
- Avoid unnecessary treatments
- Personalise your care plan
- Recognise hidden connections between symptoms
Why Genetics Matter Genes don’t tell the whole story, but they offer important clues. Some people may carry gene variants that don’t cause problems until combined with stress, illness, or another variant. We believe that one particular group of genes—the KLK (kallikrein) family—acts like an “amplifier.” Depending on what other genes you have, KLK variants might intensify inflammation, nerve sensitivity, or immune activity.
In Plain Terms: Think of KLK genes as turning up the volume on whatever song your body is already playing.
Where We’re Headed This theory is part of a larger push to better understand complex conditions like hEDS. We hope it helps:
- Patients feel validated and better understood
- Clinicians develop smarter diagnostic tools
- Researchers build clearer, testable models of hEDS
Most importantly, we want to move toward personalised, compassionate care—because every hEDS patient is different, and that difference matters.
Want to Learn More? This plain-language summary is part of a bigger project exploring hEDS as a systems-level condition. If you’re interested in the science behind these ideas, ask for our full dissertation chapters and case study models. Contact us here.
Together, we can change how hEDS is seen, studied, and treated.
Medical Disclaimer
This content is for informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your doctor or qualified health provider regarding any medical condition.
FAQ
What is Hypermobile Ehlers-Danlos Syndrome misdiagnosis?
It’s when hEDS symptoms are mistaken for other conditions like anxiety, depression, or IBS, delaying correct treatment.
Why is hEDS often misdiagnosed?
Because it affects multiple systems and lacks a definitive test, symptoms can resemble unrelated physical or mental health conditions.
How long does it take to get diagnosed with hEDS?
On average 10–12 years, sometimes longer, due to low awareness among healthcare providers.
Can the ConnectED Health App help my doctor diagnose hEDS?
While not a diagnostic tool, it provides a structured symptom report to support the diagnostic
process.
What other conditions are linked with hEDS?
Common overlaps include POTS, MCAS, neurodivergence, and post-viral syndromes like Long COVID.
About the Author
Tracy Finnegan, RN, BAppSc is the Founder and Managing Director of ConnectED. A former ICU nurse and scientist, Tracy has lived experience with hEDS, POTS, MCAS, and Long COVID. After decades of misdiagnoses, she created the ConnectED Health App to empower patients to track symptoms, identify patterns, and advocate for accurate diagnoses and better care. Tracy brings firsthand experience, clinical expertise, and a patient-focused tool to support others.


